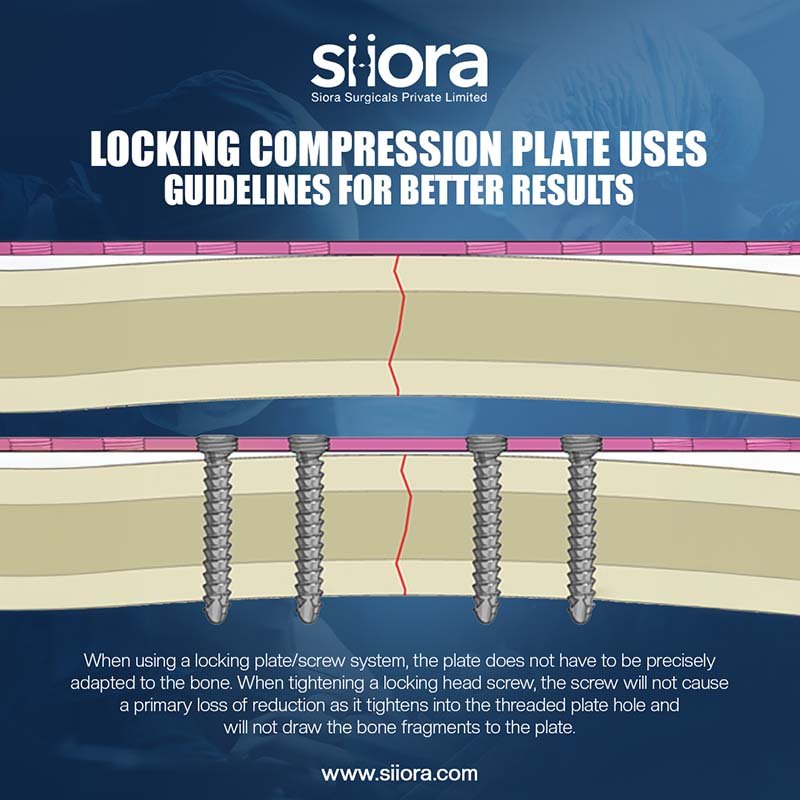
The following are some general guidelines when using these implants for Locking compression plate-LCP
- Whenever possible, the fracture is first reduced by indirect means.
- If required, the reduction is then maintained using external fixators or distractors.
- If a well-contoured or anatomically preshaped plate is utilized, the implant may be used as a reduction aid when utilized with standard screws.
- If the compression purpose of the LCP is to be utilized, for example in simple transverse fractures, correct contouring of the plate is first performed; axial compression may then be carried out utilizing standard screws in the dynamic compression unit of the combination holes. It’s significant to note that the Locking Compression Plate combination holes are arranged asymmetrically on the plate. This asymmetry enables axial dynamic compression to be exerted unidirectionally. After exerting axial compression by the standard screws, further LHS may then be inserted.
- If it’s desired to apply interfragmentary compression in a spiral or simple oblique fractures, this should first be accomplished utilizing standard screws as lag screws prior to the application of LHS.
- To insert standard screws, the universal drill guide is utilized. The screw holes are predrilled, either eccentrically or neutrally, depending on the screw’s intended function. The depth of the screw hole is then measured as well as the tap, and the suitable standard screw inserted.
- If plate contouring is required, it should be performed using suitable bending instruments. Bending should be done between the combination holes and not done through the holes. This can cause deformation of the holes and lead to difficulty in the following insertion of LHS. One way of preventing this deformation is to insert an LHS or a threaded drill sleeve into the threaded portion of the combination hole before carrying out the bending.
- If wanted, an LCP spacer is screwed into the plate before its insertion. The spacer ensures a gap of 2 mm between the plate and underlying cortex. Thus, minimizing plate-bone contact and preserving periosteal circulation. This spacer may be removed after insertion of the LHS.
- Skin incisions are made, corresponding in location to the ends of the plate.
- A tunneler can be used to create a submuscular extra-periosteal tunnel for the locking bone plate.
- The bone plate is then passed into the tunnel. This may be done in one of many ways. If a tunneler is utilized, one end of the plate is tied with a suture to the end of the tunneler. As the tunneler is withdrawn, the bone plate is pulled into position. Another way is to fix the plate’s one end with a plate holder or a threaded LCP drill guide. Which is then utilized to guide the plate into position along the track made by the tunneler.
- Once the plate is in place, bone screw insertion may follow. If the first inserted bone screw is an LHS, before locking, the other end of the plate should be temporarily stabilized with either a standard screw, a K-wire, a threaded LCP drill guide, or another LHS that isn’t locked. This is to avoid the plate from rotating and causing damage to the surrounding soft tissue as the 1st LHS is tightened and locked.
- If the equal of fracture reduction is satisfactory, the rest of the LHS is inserted.
- To insert a self-tapping LHS percutaneously, a threaded LCP drill guide is 1st introduced through a stab incision in the skin and then screwed into the threaded part of the selected combination hole. The drill guide makes sure that drilling is done in an accurate direction. Hence, the screw is appropriately locked to attain maximal angular stability. The screw hole is then drilled and measured, and the suitable LHS inserted, first utilizing a power tool with the screwdriver shaft and then performing the final tightening by hand with the torque-limiting until clicking happens.
- Predrilling and depth measurement aren’t essential if a self-drilling, self-tapping LHS is used monocortically. This, though, is only possible in good-quality bone with a thick cortex. Monocortical screw fixation is also specified in periprosthetic fractures.