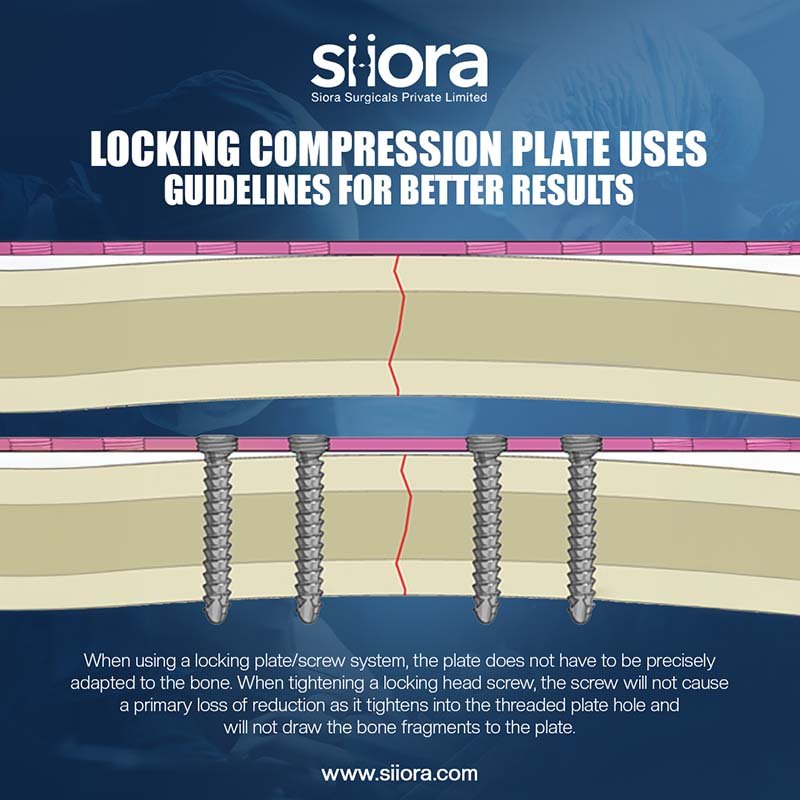
Locking Compression Plate Uses – Guidelines for Better Results
Orthopedic trauma care has made remarkable progress over the past few decades, especially in the realm of internal fixation devices. Among these innovations, the Locking Compression Plate (LCP) has emerged…