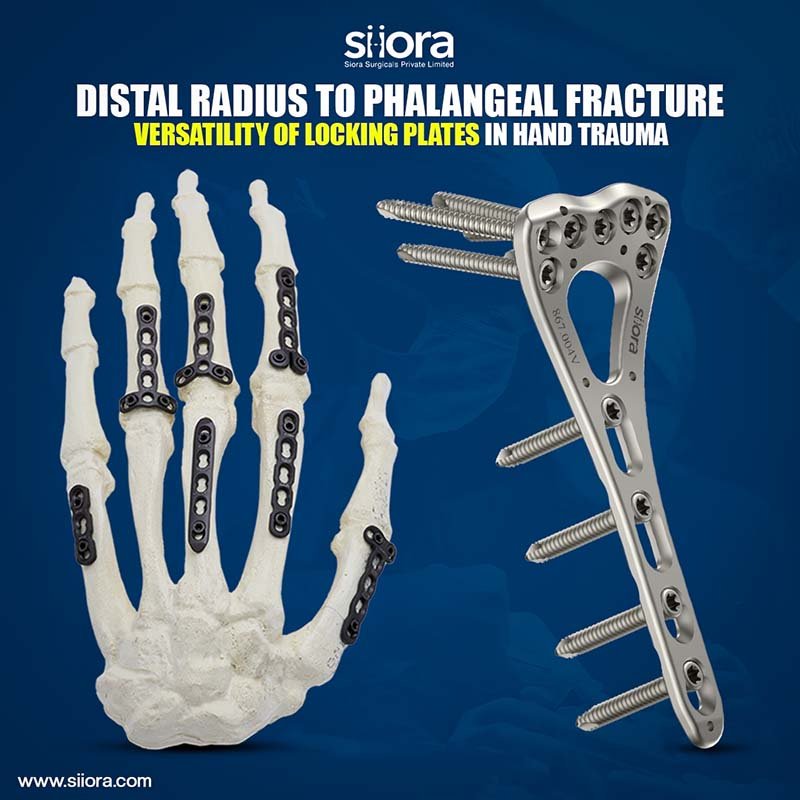
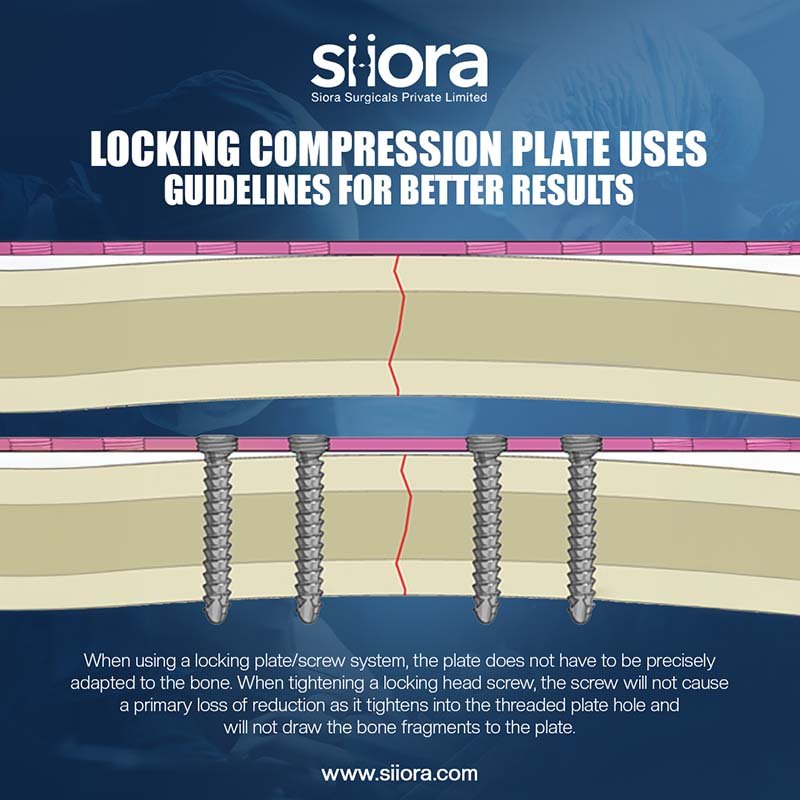
Ankle fractures are a common orthopedic injury, often requiring surgical intervention to ensure proper healing and stability. In many cases, hardware such as plates, screws, or rods is used during surgery to align and secure the broken bones. While these implants are typically designed to remain in the body permanently, there are instances where hardware removal becomes necessary or desirable. In this blog, we will explore what hardware removal entails, treatment options for ankle fracture, the precautions to take if removal is pursued, and insights into symptoms and recovery timelines.
What Is Hardware Removal After Foot or Ankle Fracture Surgery?
Hardware removal refers to a surgical procedure where previously implanted metal devices, such as screws, pins, or plates, are extracted from the foot or ankle after a fracture has healed. These devices are initially inserted to stabilize the bones during recovery and are often made of materials like stainless steel or titanium.
While hardware is usually left in place indefinitely, it may be removed for various reasons, including:
- Persistent pain or irritation near the hardware site
- Infection around the implant
- Hardware becoming loose or migrating
- Allergic reaction (rare)
- Patient preference for personal or occupational reasons (e.g., athletes, military personnel)
The decision to remove hardware is based on a combination of symptoms, diagnostic imaging, and a thorough consultation with your orthopedic surgeon.
What is the Treatment for Ankle Fracture Injuries?
Treatment for ankle injuries depends on the type and the severity. Common ankle injuries include sprains, fractures, and tendon or ligament tears. Treatment options include:
Conservative Treatment
- Rest, Ice, Compression, Elevation (RICE): Initial approach for mild injuries.
- Bracing or Splinting: Used to immobilize the joint and allow healing.
- Physical Therapy: Helps restore strength, mobility, and function.
Surgical Treatment
- Open Reduction and Internal Fixation (ORIF): ORIF is often used for moderate to severe fractures. The surgeon realigns the bones and uses hardware to stabilize them.
- Ligament Repair or Reconstruction: Required in cases of significant ligament damage.
Surgery is typically followed by a structured rehabilitation program to regain full mobility and strength.
Do I Need to Take Precautions if I Decide to Have Hardware Removed?
Yes, if you and your surgeon decide on hardware removal, it is important to take certain precautions before and after the procedure.
Before Surgery
- Health Evaluation: Make sure that you are medically fit for surgery. Inform your doctor of any underlying conditions.
- Imaging Tests: X-rays or MRIs will help assess healing and guide surgical planning.
- Medication Review: You may need to stop some medications before surgery, especially blood thinners.
After Surgery
- Rest and Elevation: You should keep the operated leg elevated to minimize swelling.
- Limited Weight Bearing: You may need to use crutches or a walker temporarily.
- Wound Care: Keep the incision area clean and dry to prevent infection.
- Follow-up Visits: Regular check-ups are essential to monitor healing.
- Physical Therapy: Rehab exercises will help restore movement and strength.
Although hardware removal is usually less complex than the initial fracture surgery, recovery still requires time and care.
What Are Ankle Fracture Symptoms?
Recognizing the symptoms of an ankle fracture is crucial for timely treatment. Common signs include:
- Severe pain: Especially while bearing weight or moving the ankle.
- Swelling and bruising: Around the ankle and foot.
- Deformity: In severe cases, the ankle may appear out of place.
- Tenderness: When pressing on the injured area.
- Inability to walk: Or difficulty putting weight on the foot.
Above all, it is essential to seek medical attention if you experience any of these symptoms after a fall or twist of the ankle.
What is Ankle Fracture Recovery Time?
The recovery timeline for an ankle fracture can vary based on the injury’s severity and the type of treatment involved.
Non-Surgical Recovery
- 6 to 8 weeks: For mild fractures treated with immobilization.
- Physical therapy may continue for another 4-6 weeks to regain full mobility.
Surgical Recovery (with hardware)
- Initial healing (bone union): Typically takes 6 to 12 weeks.
- Return to normal activity: May take 3 to 6 months.
- Full recovery: Including strength and range of motion, can take up to a year in some cases.
Following your surgeon’s recommendations and staying consistent with rehabilitation are key factors for a successful recovery.
Conclusion
Not every patient with an ankle fracture that was treated with hardware will need the implants removed. In many cases, the hardware causes no issues and remains in the body without complication. However, if you experience pain, irritation, or other concerns, hardware removal may be a beneficial option. Consulting with your orthopedic specialist is the best way to determine the most appropriate course of action for your specific condition. At last, with proper care, whether you keep or remove the hardware, you can look forward to a full and functional recovery.